|
Case Report
Mesh migration – Should it be a mandatory consentable complication?
1 Surgical Trainee, General Surgery, Aberdeen Royal Infirmary, Aberdeen, UK; 2StR General Surgery, Aberdeen Royal Infirmary, Aberdeen, UK
2 StR General Surgery, Aberdeen Royal Infirmary, Aberdeen, UK
3 Consultant General Surgeon, Aberdeen Royal Infirmary, Aberdeen, UK
Address correspondence to:
Pia Persson
Colorectal Department, Aberdeen Royal Infirmary, Foresterhill, Aberdeen, AB25 2ZN,
UK
Message to Corresponding Author
Article ID: 100057Z12PP2019
Access full text article on other devices

Access PDF of article on other devices

How to cite this article
Persson P, Scrimgeour DSG, Parnaby C. Mesh migration – Should it be a mandatory consentable complication? J Case Rep Images Surg 2019;5:100057Z12PP2019.ABSTRACT
Introduction: Use of mesh in hernia repair is becoming more prevalent, particularly with new evidence supporting mesh repair over suture repair for even small ventral hernias to reduce recurrence. There is an acknowledgement that mesh-related complication rates are currently poorly reported and there is a need for improvement. Public awareness of complications due to the use of mesh in surgery is also increasing, particularly with the rise in complications associated with vaginal meshes documented in the press.
Case Report: We describe one of only a few cases reported in the literature of mesh migration into the transverse colon several years after laparoscopic repair of an incisional ventral hernia, and discuss whether mesh migration should be a mandatory consentable complication.
Conclusion: Consequences of mesh migration are undoubtedly severe, often resulting in symptoms including chronic abdominal pain, bowel obstruction, or fistulae formation, all of which may require significant surgical intervention. We feel surgeons should include mesh migration and its potential complications as part of the consent process.
Keywords: Consent, Hernia, Mesh, Mesh complications
Introduction
There are many different types of mesh available for hernia repair and they can be broadly categorized into synthetic, biological and absorbable or permanent composite meshes [1]. Their use in hernia repair is becoming more prevalent, particularly with new evidence supporting mesh repair over suture repair for even small ventral hernias [2]. With the long-term complications from vaginal meshes only recently becoming apparent, it has been suggested that the use of any implant should be recorded on a national, if not international, database so that complications can be identified at an early stage [3]. The UK government has recently created a prospective registry for vaginal mesh whilst simultaneously conducting a retrospective audit [4]. However, as investment increases in mesh research, the numbers of different licensed meshes on the market for hernia repair is likely to increase, making analysis more complicated. We describe one of only a few cases reported in the literature of mesh migration into the transverse colon several years after laparoscopic repair of an incisional ventral hernia, and discuss whether mesh migration should be a mandatory consentable complication.
Case Report
A 78-year-old woman with an extensive past medical history including Type 2 diabetes mellitus and obesity presented as an emergency with gradually worsening abdominal pain, constipation, weight loss and failure to thrive over a two-month period. In 2012 (6 years prior to presentation) she developed a symptomatic ventral incisional hernia and underwent a laparoscopic intraperitoneal onlay mesh repair with a 20 cm x 30 cm intracorporeal ParietexTM Composite mesh (Covidien AG, New Haven, CT, USA). An AbsorbaTackTM (Covidien AG) fixation device was used to secure the mesh over the defect. There were no intraoperative or immediate postoperative complications, and the patient was discharged home the following day. Her past surgical history included previous laparotomies: appendicectomy (1975), cholecystectomy (1978), adhesiolysis for small bowel obstruction (1999) and a sigmoid colectomy for stricturing diverticular disease (2010).
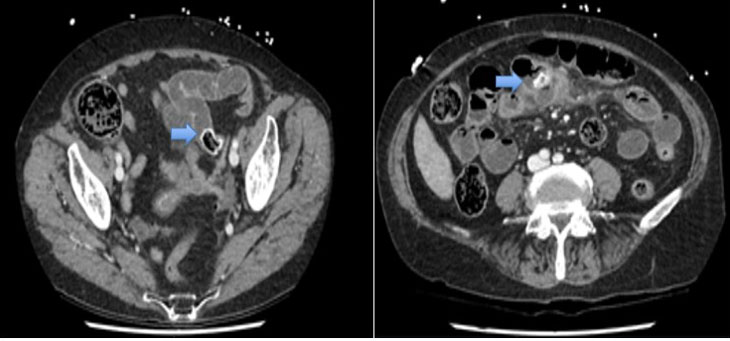
On examination, she was found to have a tender mass over her midline laparotomy incision and an urgent CT scan was arranged. This revealed an ill-defined highdensity foreign body in the mid-transverse colon (Figure 1). There was associated thickening of the transverse colon and marked inflammatory changes which extended into the anterior abdominal wall around the umbilical region. A 4.8 cm gas and fluid collection was reported inferior to this segment of transverse colon with several loops of adherent small bowel identified. There was no evidence of small or large bowel obstruction.
A decision was made for surgical intervention. At time of midline laparotomy, a large mass was found adherent to the anterior abdominal wall containing the hernial sac, most of the ileum and some jejunum. The mesh was found to have eroded into the transverse colon (Figure 1). The mass was mobilised en-bloc following excision of the abdominal wall beyond the lateral border of the left rectus muscle. A length of involved small bowel was also resected along with a wedge of the transverse colon and mesh at the site of the perforation. An end to end jejunoileal anastomosis was performed and a loop colostomy was fashioned using the site of the wedge resection. Due to the large size of the inflammatory mass and its fusion to the abdominal wall, a posterior component separation with bilateral transversus abdominis muscle release was required to approximate the midline.
Post-operatively the patient had a prolonged recovery in the surgical high dependency unit but was discharged on postoperative day 14 to a community hospital for ongoing rehabilitation. She made a full recovery. Four months postoperatively the midline wound has healed and there is no evidence of hernia recurrence.
Discussion
In 1992, LeBlanc and Booth introduced laparoscopic ventral incisional hernia repair into surgical practice [5]. They described a method using expanded polytetrafluoroethylene patches with staples to secure the mesh, similar to the intraperitoneal onlay mesh (IPOM) technique commonly used today. Laparoscopic repair has been shown to have many benefits over open repair including a reduced incidence of wound infections and similar rates of hernia recurrence [6]. There are also the advantages of shorter hospital stay and recovery times. Since the 1990s there have been multiple reviews comparing laparoscopic versus open mesh repair but a recent meta-analysis and systematic review of elective mesh repair of incisional hernias in 2015 concluded that both techniques were comparable [7]. Laparoscopic IPOM repair may be of benefit for large ventral hernias, particularly in patients with comorbidities including factors affecting wound healing such as diabetes and obesity. IPOM repair may have a higher rate of mesh migration as the mesh is attached directly to the peritoneum rather than the transversalis fascia [8].
The most effective method of mesh fixation is also widely disputed. Despite the popularity of tack fixation, a recent meta-analysis and systematic review of 6553 cases of laparoscopic ventral hernia repair found that fixation with sutures had a 93% chance of having fewer complications, compared to other techniques, but this did not reach statistical significance [9]. It has also been suggested that suture fixation may increase the risk of post-operative pain, wound infection and increase operating time, and manufactures of absorbable tacks often quote reduced post-operative pain and seroma formation [10].
Mesh migration, as described in our case report, is rare but can cause severe morbidity. A study in 2005 looked at 252 adverse event reports involving surgical mesh for abdominal wall hernia repairs [11]. The authors found an incidence of 2% for mesh migration, and 7% for intestinal complications. Picchio et al. found 8 case reports of complete transmural mesh migration in a literature review in 2017, all resulting in severe morbidity and presenting up to 14 years following initial repair [12].
Public awareness of complications due to the use of mesh in surgery is also increasing, particularly with the rise in medical litigation and the recognition of long-term complications associated with synthetic trans-vaginal meshes [13]. The recognition of complications with the use of mesh for hernia repair has also increased due to the recall of meshes, such as the Kugel® mesh implants by Bard Davol. An estimated 350 000 units were used between its introduction in 2000 and recall in 2005, however the estimated risk of mesh breakage is reported at 0.009% [14].
During informed consent both common and potentially severe but rare complications must be discussed with each patient prior to any surgical procedure. Rare complications addressed during consent for any surgery varies widely between surgeons. The American College of Surgeons has a patient education brochure detailing risks patients should be aware of before undergoing a ventral hernia repair [15]. The risks listed include: urinary retention, urinary tract infection, seroma, recurrence, bowel injury, wound infection, return to theatre, pneumonia, venous thromboembolism, cardiac complications, renal failure and death. A recent study in the Hernia journal of UK NHS trusts on consent for groin hernias reported that only 14% of trusts use pre-printed consent forms which listed 28 different risks [16]. Mesh migration was not listed on any forms. Mesh migration is likely to have a much higher incidence than reported due to delayed presentation and under reporting. In our case, there was a delay of six years between hernia repair and presentation to the surgical department. There is an acknowledgement that mesh related complication rates are currently poorly reported and there is a need for improvement [17]. Many sources have called for a UK mesh register to accurately collect mesh related complications across all surgical specialities [4],[18]. A voluntary registry, EuraHS, has already been developed for ventral abdominal wall hernia repair across Europe [19].
Conclusion
Consequences of mesh migration are undoubtedly severe, often resulting in symptoms including chronic abdominal pain, bowel obstruction, or fistulae formation, all of which may require significant surgical intervention. For these reasons, we feel surgeons should include mesh migration and its potential complications as part of the consent process. It is also vital to consider mesh migration as a differential diagnosis in all patients who present acutely or many years after surgery who have a background of previous hernia repair with mesh.
REFERENCES
1.
Bilsel Y, Abci I. The search for ideal hernia repair; mesh materials and types. Int J Surg 2012;10(6):317–21. [CrossRef]
[Pubmed]

2.
Kaufmann R, Halm JA, Eker HH, et al. Mesh versus suture repair of umbilical hernia in adults: A randomised, double-blind, controlled, multicentre trial. Lancet 2018;391(10123):860–9. [CrossRef]
[Pubmed]

3.
Köckerling F, Simon T, Hukauf M. The importance of registries in the postmarketing surveillance of surgical meshes. Ann Surg 2018;268(6):1097–104. [CrossRef]
[Pubmed]

4.
Heneghan C, Godlee F. Surgical mesh and patient safety. BMJ 2018;363:k4231. [CrossRef]
[Pubmed]

5.
LeBlanc KA, Booth WV. Laparoscopic repair of incisional abdominal hernias using expanded polytetrafluoroethylene: Preliminary findings. Surg Laparosc Endosc 1993;3(1):39–41.
[Pubmed]

6.
Al Chalabi H, Larkin J, Mehigan B, McCormick P. A systematic review of laparoscopic versus open abdominal incisional hernia repair, with meta-analysis of randomized controlled trials. Int J Surg 2015;20:65–74. [CrossRef]
[Pubmed]

7.
Awaiz A, Rahman F, Hossain MB, et al. Meta-analysis and systematic review of laparoscopic versus open mesh repair for elective incisional hernia. Hernia 2015;19(3):449–63. [CrossRef]
[Pubmed]

8.
Yang GPC. From intraperitoneal onlay mesh repair to preperitoneal onlay mesh repair. Asian J Endosc Surg 2017;10(2):119–27. [CrossRef]
[Pubmed]

9.
Baker JJ, Öberg S, Andresen K, Klausen TW, Rosenberg J. Systematic review and network meta-analysis of methods of mesh fixation during laparoscopic ventral hernia repair. Br J Surg 2018;105(1):37–47. [CrossRef]
[Pubmed]

10.
Zahiri HR, Belyansky I. Evidence-based optimal fixation during laparoscopic hernia repair: Sutures, tacks, and glues. In: Novitsky Y, editor. Hernia Surgery. Cham: Springer International Publishing; 2016. p. 287–95. [CrossRef]

11.
Robinson TN, Clarke JH, Schoen J, Walsh MD. Major mesh-related complications following hernia repair. Surg Endosc 2005;19(12):1556–60. [CrossRef]
[Pubmed]

12.
Picchio M, Muggianu A, Mancini F, Tintisona O, Spaziani E. Complete mesh migration into the small bowel after incisional hernia repair: A case report and literature review. Acta Chir Belg 2017;117(2):118–21. [CrossRef]
[Pubmed]

13.
Menchen LC, Wein AJ, Smith AL. An appraisal of the food and drug administration warning on urogynecologic surgical mesh. Curr Urol Rep 2012;13(3):231–9. [CrossRef]
[Pubmed]

14.
Hope WW, Iannitti DA. An algorithm for managing patients who have Composix® Kugel® ventral hernia mesh. Hernia 2009;13(5):475–9. [CrossRef]
[Pubmed]

15.
Felicano D, Hawn MT, Strand N, Heneghan K. Patient Education - Ventral Hernia Repair. Chicago. 2017. [Available at: https://www.facs.org/~/media/files/education/patient%20ed/ventral_hernia.ashx]

16.
Courtney MJ, Royle TJ. Pre-made consent for elective inguinal hernia repair: The need for standardisation—a survey of all UK NHS Trusts. Hernia 2018;22(3):549–53. [CrossRef]
[Pubmed]

17.
Ratajczak A, Ko?ci?ski T, Banasiewicz T, et al. Migration of biomaterials used in gastroenterological surgery. Pol Przegl Chir 2013;85(7):377–80. [CrossRef]
[Pubmed]

18.
Gornall J. How mesh became a four letter word. BMJ 2018;363:k4137. [CrossRef]
[Pubmed]

19.
Muysoms F, Campanelli G, Champault GG, et al. EuraHS: The development of an international online platform for registration and outcome measurement of ventral abdominal wall hernia repair. Hernia 2012;16(3):239–50. [CrossRef]
[Pubmed]

SUPPORTING INFORMATION
Author Contributions
Pia Persson - Substantial contributions to conception and design, Acquisition of data, Analysis of data, Interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published
Duncan S GS crimgeour - Substantial contributions to conception and design, Revising it critically for important intellectual content, Final approval of the version to be published
Craig Parnaby - Revising it critically for important intellectual content, Final approval of the version to be published
Guarantor of SubmissionThe corresponding author is the guarantor of submission.
Source of SupportNone
Consent StatementWritten informed consent was obtained from the patient for publication of this case report.
Data AvailabilityAll relevant data are within the paper and its Supporting Information files.
Conflict of InterestAuthors declare no conflict of interest.
Copyright© 2019 Pia Persson et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information.