|
Case Report
Rectal perforation secondary to carcinosarcoma of gynecological origin
1 Acute Surgical Unit, The Canberra Hospital, Yamba Drive, Garran, ACT 2605, Australia
Address correspondence to:
Natalie Quarmby
Acute Surgical Unit, The Canberra Hospital, Yamba Drive, Garran, ACT 2605,
Australia
Message to Corresponding Author
Article ID: 100116Z12NQ2023
Access full text article on other devices

Access PDF of article on other devices

How to cite this article
Quarmby N, Balasooriya J. Rectal perforation secondary to carcinosarcoma of gynecological origin. J Case Rep Images Surg 2023;9(1):4–8.ABSTRACT
Introduction: Carcinosarcoma is an aggressive, rare tumor containing both epithelial and stromal elements that can be found in the female genital tract. Colorectal perforation resulting from this is a highly unusual occurrence, with poor prognosis for affected patients.
Case Report: This is the case of an 86-year-old lady who presented with a history of rectal bleeding, abdominal distention and recent unintentional weight loss. She was subsequently found to have a large rectal perforation with associated abscess secondary to a new diagnosis of a rare, high grade carcinosarcoma of ovarian or gynecological tract origin. Following a trial of conservative management, the patient underwent formation of a colostomy and was palliated post-operatively due to severe aspiration pneumonia.
Conclusion: While perforation of the colon or rectum secondary to ovarian or gynecological malignancy including carcinosarcoma is rare, it is an important diagnosis to consider in patients who present with known or suspected malignancy and associated features of sepsis.
Keywords: Carcinosarcoma, Gynecological malignancy, Rectal perforation
Introduction
Carcinosarcoma is a rare and aggressive tumor, which associates some epithelial elements with a stromal component and can be found in the female genital tract, mostly in the uterus, although rarely also arising from the ovaries. In addition to this, colorectal perforation secondary to invasion by ovarian or gynecological malignancy, without an associated history of chemotherapy or radiotherapy is also extremely rare [1]. Here, we report the case of an 86-year-old lady who presented with a history of rectal bleeding, abdominal distention, and recent unintentional weight loss, who was subsequently found to have a large rectal perforation with associated abscess secondary to a new diagnosis of a rare, high grade carcinosarcoma of ovarian or gynecological tract origin.
Case Report
An 86-year-old lady was brought in by ambulance to the emergency department with a 2-week history of rectal bleeding and abdominal distention, which was associated with fatigue, nausea, and recent unintentional weight loss. Her past medical history consisted of cutaneous follicle center lymphoma, rheumatoid arthritis, and hypertension. Her surgical history included bilateral salpingectomy and she had undergone a colonoscopy five years prior demonstrating polyps and diverticulosis.
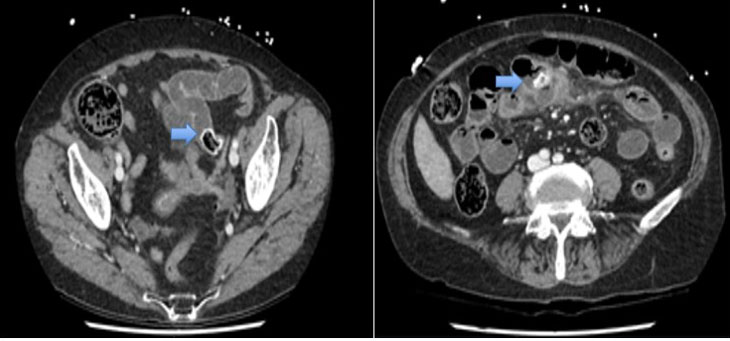
On arrival, she was tachycardic [heart rate (HR) 110 bpm], normotensive, and afebrile. On examination her abdomen was tender in the left lower quadrant and suprapubic regions. Despite baseline continence, the patient was noted to have constant fecal ooze from the rectum, with red blood and feces found on internal rectal examination. Blood tests demonstrated a hemoglobin of 8.3 g/dL and white cell count of 17.5×109/L, with a lactate of 3.3 mmol/L. Computed tomography (CT) angiogram was performed on admission which demonstrated large volume ascites, extensive colonic fecal loading, and suggestion of collapsed and thickened distal sigmoid colon and rectum with no discrete bowel mass identified. In the posterior pelvis/presacral region, there was a large fluid and gas containing collection with thick enhancing walls measuring approximately 97×111×89 mm of unclear origin (Figure 1). Immediate management consisted of transfusing 1 unit of packed red blood cells and commencement on intravenous antibiotics (Ceftriaxone and Metronidazole). Blood cultures taken at the time of admission grew Clostridium perfringens and Escheria coli. Her Ca-125 markers were found to be elevated to 223 U/mL.
Magnetic resonance imaging (MRI) scan was obtained at this time which demonstrated a large heterogenous mass between the bladder and the rectum measuring 8×8×9 cm, thought to be uterine in origin and compressing the rectum causing large bowel obstruction (Figure 2). A large locule of air was suggestive of perforation of the rectosigmoid junction into the mass. The patient was not clinically obstructed, and improvement was noted with intravenous antibiotics initially. Considering the thickness of the fluid, imaging guided drainage was not attempted. Subsequent CT with rectal contrast demonstrated most of the contrast emptying from the rectosigmoid junction into a large extra-luminal collection with an air-fluid level and fecalized material. The rectosigmoid defect was large, measuring 4.1 cm with a lobulated soft tissue mass within and inferior to the large collection measuring 9.5×6.9×7.8 cm (Figure 3). There was also a dominant pelvic collection measuring up to 13 cm in maximal diameter, occupying most of the pelvis, with gas in it.
Based on the imaging findings and the overall clinical picture, extensive discussion was held with the patient and family, and the decision was made to perform an exploratory laparotomy. A lower midline laparotomy was performed. A large pelvic collection was drained and fecal material evacuated. Associated necrotic tissue was debrided and sent for histology. The upper rectum where the perforation was located was unable to be mobilized due to dense inflammatory adhesions and unclear underlying pathology. No obvious malignant mass was identified. Although a Hartmann’s procedure is preferred (rectosigmoid resection, closure of rectal stump and formation of colostomy), due to the above reasons a de-functioning loop colostomy was formed following mobilization of the descending colon. A 19 French Blake drain was left in the pelvis, and the patient was continued on intravenous (IV) antibiotic therapy.
The patient initially progressed well post-operatively and was tolerating full diet with a functioning stoma; however, later aspirated resulting in a severe pneumonia on the ward and was subsequently palliated and died on day 5 post-operatively.
Histopathology was identified as a high grade carcinosarcoma, consistent with an ovarian/gynecological tract origin, and an associated pelvic abscess, necrotic debris, inflammation, and vegetable material (Figure 4). The immunohistochemistry showed that the cells were weak-moderately positive for CK7 and were positive for P16 and P53 stains (Figure 5). The WT1 stain was also positive.
Discussion
Ovarian cancer is one of the most common gynecological malignancies affecting women, with an insidious clinical onset due to subacute and non-specific symptoms [2]. Carcinosarcoma is a rare subgroup of this disease, comprising less than 5% of cases, and made up of malignant epithelial and malignant mesenchymal cell populations [3],[4]. The majority have been found to be WT1 positive with aberrant p53 expression patterns, as can be seen with the patient in this case [4]. These malignancies often present in the older population with late-stage disease and subsequent poor prognosis, however, tend to remain within peritoneal planes, and therefore colorectal perforation is exceedingly rare despite anatomical proximity and invasion into the wall, with less than 10 cases reported in the literature, mostly presenting as fistulas and abscesses of small size [1],[5],[6]. One study reports a frequency of less than 1% [7]. Most often patients with these malignancies present with abdominal pain, distention, nausea, and vomiting, as seen with this patient [5]. There may be associated alteration in bowel movements; however, this is rare [6]. The cause of fistulous communication in cases of ovarian malignant tumor is considered to be a combination of chronic inflammation or leakage of cystic fluid and the subsequent invasion of malignant cells, potentially due to underlying conditions such as endometriosis [5],[8]. More often, perforation in gynecological malignancy occurs during chemotherapy, particularly with the use of anti-angiogenic agents such as Bevacizumab [2],[6],[9]. A diagnosis of perforation should be considered in patients with known or suspected ovarian malignancy who develop sepsis or an acute abdomen, with early diagnosis and management imperative to successful treatment, often reliant upon the use of CT [1],[5]. Diagnosis may also require the use of a barium enema to adequately characterize the perforation or fistula formation, as was the case for this patient [5]. Intestinal perforation is generally considered to be an emergent condition with a high associated mortality rate [6]. The perforation can result in spillage of intestinal contents resulting in peritonitis, intra-abdominal abscess, or both, and therefore has a high associated mortality rate [6]. If the leak is walled off, then emergent surgery may not be required. However, in more severe cases, the patient may require surgical or radiologically guided drainage of a small collection, or more significant surgical intervention may be required including en-bloc resection of the tumor and rectosigmoid colon and/or the formation of a stoma [1],[6]. In our case, non-operative management was done with intravenous fluid therapy and antibiotics considering the initial stable hemodynamic status of the patient and symptomatic improvement that occurred with conservative treatment. Surgery was offered following demonstration of the large rectal defect and the extension of the collection containing gas.
One study identified that compared to surgical treatment, conservative management of perforation was associated with significantly shorter survival (11.43 months vs 1.93 months, p=0.02), as was an extensive cancer burden at the time of perforation [6]. Length of hospital stay and rate of admission to the intensive care unit was found to be significantly longer in patients who underwent surgery [6]. Although both primary cytoreductive surgery and disease stage have been reported as significant prognostic factors, this was decided against at the time of surgery, and a loop colostomy formed as there was no confirmed diagnosis of a malignancy and due to extensive inflammatory changes following perforation, the surgical risk was considered very high [4],[6].
Conclusion
While perforation of the colon or rectum secondary to ovarian or gynecological malignancy including carcinosarcoma is rare, it is an important diagnosis to consider in patients who present with known or suspected gynecological or ovarian malignancy with features of sepsis.
REFERENCES
1.
Bats AS, Rockall AG, Singh N, Reznek RH, Jeyarajah A. Perforation of a malignant ovarian tumor into the recto-sigmoid colon. Acta Obstet Gynecol Scand 2010;89(10):1362–3. [CrossRef]
[Pubmed]

2.
Pitarch-Martínez M, Blanco-Elena JA, Robles-Quesada MT, Alberca-Páramo A, Granados-García J. Colonic perforation due to ovarian cancer invasion: An unusual event. Int J Gynaecol Obstet 2021;154(3):574–5. [CrossRef]
[Pubmed]

3.
Kord A, Rabiee B, Elbaz Younes I, Xie KL. Uterine carcinosarcoma: A case report and literature review. Case Rep Obstet Gynecol 2020;2020:8816348. [CrossRef]
[Pubmed]

4.
Hollis RL, Croy I, Churchman M, Bartos C, Rye T, Gourley C, Herrington CS. Ovarian carcinosarcoma is a distinct form of ovarian cancer with poorer survival compared to tubo-ovarian high-grade serous carcinoma. Br J Cancer 2022;127(6):1034–42. [CrossRef]
[Pubmed]

5.
Yahagi N, Kobayashi Y, Ohara T, Suzuki N, Kiguchi K, Ishizuka B. Ovarian carcinoma complicated by sigmoid colon fistula formation: As case report and review of the literature. J Obstet Gynaecol Res 2011;37(3):250–3. [CrossRef]
[Pubmed]

6.
Garg G, Massad LS, Pourabolghasem S, et al. Intestinal perforation in gynecologic oncology: Do all patients benefit from surgical management? Gynecol Oncol 2013;129(3):538–43. [CrossRef]
[Pubmed]

7.
Kizaki Y, Nagai T, Ohara K, et al. Ovarian mature cystic teratoma with fistula formation into the rectum: A case report. Springerplus 2016;5(1):1700. [CrossRef]
[Pubmed]

8.
Min KW, Lee SJ, Jung HY, et al. Squamous cell carcinoma arising in a mature cystic teratoma exposed through a colo-ovarian fistula. J Obstet Gynaecol 2015;35(7):763–4. [CrossRef]
[Pubmed]

9.
Schorge JO. Laparoscopic diverting loop ileostomy for spontaneous colon perforation in advanced ovarian cancer. Gynecol Oncol Rep 2019;28:84–5. [CrossRef]
[Pubmed]

SUPPORTING INFORMATION
Author Contributions
Natalie Quarmby - Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Janaka Balasooriya - Conception of the work, Design of the work, Acquisition of data, Drafting the work, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
AcknowledgmentsDr Alexander Borecki, Pathology Department, The Canberra Hospital, Yamba Drive Garran, ACT 2605.
Guarantor of SubmissionThe corresponding author is the guarantor of submission.
Source of SupportNone
Consent StatementWritten informed consent was obtained from the patient next of kin for publication of this article.
Data AvailabilityAll relevant data are within the paper and its Supporting Information files.
Conflict of InterestAuthors declare no conflict of interest.
Copyright© 2023 Natalie Quarmby et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information.