|
Case Report
Intestinal duplication in an adult presenting as acute small bowel obstruction with malrotation and volvulus: Case report and updated review of the literature
1 Attending Surgeon, Department of General Surgery, IMED Levante Hospital, Calle Dr. Santiago Ramón y Cajal, 7, 03503 Benidorm, Alicante, Spain
2 Medical Student, Rosalind Franklin University of Medicine & Sciences, Chicago Medical School, 3333 N Green Bay Rd, North Chicago, IL 60064, USA
Address correspondence to:
Marie Nunez Duarte
Chicago Medical School, Class of 2025, 3333 N Green Bay Rd, North Chicago, IL 60064,
USA
Message to Corresponding Author
Article ID: 100145Z12MG2024
Access full text article on other devices

Access PDF of article on other devices

How to cite this article
Gomez ME, Duarte MN, Silver R, Dieter A. Intestinal duplication in an adult presenting as acute small bowel obstruction with malrotation and volvulus: Case report and updated review of the literature. J Case Rep Images Surg 2024;10(2):26–31.ABSTRACT
Introduction: Intestinal malrotation and duplication are rare congenital anomalies that typically present in childhood, but can also occur in adults. Adult presentations are often associated with acute obstructive symptoms, and complications like volvulus and ischemia can rapidly lead to life-threatening outcomes. Early recognition and intervention are essential for ensuring favorable outcomes.
Case Report: We report an interesting case of intestinal duplication and malrotation in a 49-year-old male who presented with acute abdominal pain, bilious vomiting, and bloating. Imaging revealed a twisted intestinal segment, initially mimicking a large Meckel’s diverticulum. Surgical exploration uncovered an ischemic segment of ileum with complex torsion and gangrene, necessitating resection and anastomosis.
Conclusion: This case highlights the rarity of intestinal malrotation presenting in adulthood, and the severe complications that can result. The rapid progression to ischemia and necrosis emphasizes the need for timely surgical intervention. While Ladd’s procedure is often the treatment of choice, it is not feasible when bowel viability is compromised, as in this case. Adult presentations of intestinal duplication with volvulus are rare, but should be considered in patients with acute obstructive symptoms.
Keywords: Adult congenital anomalies, Intestinal duplication, Intestinal malrotation, Ischemic bowel, Small bowel obstruction, Surgical resection, Volvulus
Introduction
Intestinal duplications are cystic or tubular structures that develop with a shared common blood supply found in 1 per 4500 live births [1]. Previously, duplications were known as giant diverticula, enteric cysts, intestinal duplex, or a variation of Meckel diverticulum until the term “intestinal duplication” was popularized in the 1930s [2]. The most common site where they may be found are the ileum and jejunum, then the esophagus, stomach, and colon. Intestinal malrotation in adults has been estimated to have an incidence of 0.2–1% [3].
Males make up 60–80% of cases of intestinal duplication and a third may have associated congenital anomalies. The majority of cases present before the age of 2 years old, but many remain asymptomatic [4]. Presentations include bleeding, chronic pain, or perforation if the duplication contains heterotopic mucosa.
While the cause of intestinal duplications remain unclear, theories include a failure in recanalization, a vascular insult, persistence of embryonic diverticula, and partial twinning. Currently, surgical resection is still the mainstay of treatment. The results form a systematic search of the literature is shown in Table 1. We aim to compare our patient’s clinical data and associated previous studies to further elucidate the diagnosis and potential treatment options.
Case Report
A 49-year-old male patient presented to urgent care 4 hours following the onset of abdominal pain severe enough to awaken him from sleep. He also reported bilious vomiting and bloating.
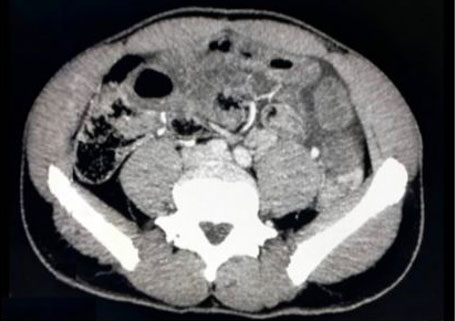
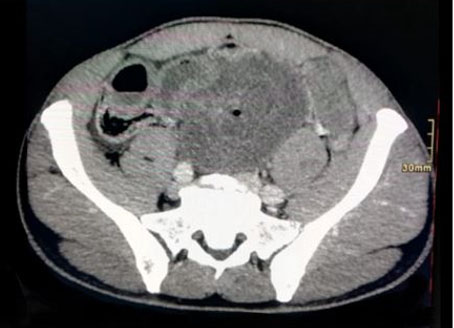
A computed tomography (CT) of the abdomen and pelvis was obtained, showed dilated thin loops of bowel in the meso- and hypogastrium, full of liquid, and with a thickened wall surrounding engorged mesenteric vessels, forming the swirl sign, compatible with small bowel obstruction and volvulus (Figure 1 and Figure 2).
A supra/infraumbilical median laparotomy was performed. During surgical exploration, an ischemic segment of the ileum was appreciated arising adjacent to the ileocecal valve, initially giving the appearance of a large Meckel’s diverticulum. This segment of small bowel included the appendix and was herniated through an internal hernia orifice in the ileal mesentery, with complex torsion and gangrene, but no perforation (Figure 3).
Devolvulation in a counterclockwise direction followed, then dissection and section with the Voyant sealing device. The ascending colon was exposed via the Toldt’s fascia. The healthy bowel loops were connected with the proximal end 3 meters from the ligament of Treitz and the distal end at the cecal pole. A linear anastomosis with gastrointestinal anastomosis (GIA) was completed and reinforced with stitches on the anterior surface of the anastomosis. Endoluminal hemorrhage was appreciated in the specimen that was sent for frozen section. An intraoperative diagnosis of intestinal duplication, obstruction, and volvulus was made. In total, the operative time was 1 hour.
The specimen was found to be a 75 cm long intestinal segment with transmural, coagulative necrosis, without evidence of malignancy or epithelial dysplasia. The cecal appendix measured 1.5 cm and was without histological lesions. The perivisceral adipose tissue also showed mixed ischemic and hemorrhagic necrosis. Lymph nodes were without injury.
Postoperatively, the patient spent less than 24 hours in the intensive care unit (ICU). After transferring to the floor, he had normoactive bowel sounds and was started on early oral feeds. On postoperative day (POD) 2 he was found to have mild abdominal distention, bright red rectal hemorrhage mixed with melena. His vitals remained stable. On POD 3, a CT angiogram was ordered, which was negative for active bleeding, with an intact anastomosis. Hemoglobin trended upward without the need for transfusion. Postoperative ileus was also appreciated and resolved without intervention. The patient was discharged on POD 7.
Discussion
This is a rare presentation of intestinal malrotation in an adult with only 23 cases reported in a systematic review on the subject as of 2018. It is quite rare for intestinal malrotations to remain asymptomatic until adulthood; most present with obstruction or bleeding before the age of two [5],[6]. Our case was unique due to the size of the defect, rapid progression from the onset of symptoms to ischemia and necrosis of the small intestine.
Adults with congenital intestinal malrotation may present with an acute abdomen and even strangulation or necrosis [7]. Ladd’s procedure allows for the broadening of the mesentery and lysis of Ladd’s bands, positioning the bowel in a non-rotated position. A non-rotated position is one where the small bowel is on the right and the large bowel is on the left. However, this procedure can only be performed if the intestinal segment remains viable. Surgical resection and anastomosis, as in our case and as reported in 17 others, remains the cornerstone of management due to tissue necrosis and concerns for malignancy [5],[8],[9]. Two cases of duodenal duplication were managed endoscopically; one with hemoclipping and another with drainage [10],[11].
Surgical management leads to exceptional outcomes in the majority of cases. Seventeen of the patients described in the literature were discharged within days of their surgery without major complications, similarly to our case, and with relatively no impact on their daily functioning [6],[8],[10],[12],[13],[14],[15],[16],[17],[18],[19],[20]. Two patients required a stoma due to extensive tissue necrosis, although one was able to be reversed three months later [12],[21]. This is likely due to the fact that most patients were largely in good health prior to developing abdominal issues, and over half were under the age of 40.
Conclusion
A high index of suspicion must be maintained for intestinal duplication in the acute development of obstructive symptoms for adult patients who fit the clinical picture and, in particular, patients with associated congenital conditions.
Our case was unique because of the length of torsioned intestine and rapid progression to ischemia and necrosis. While there is no current standard of practice regarding adult congenital intestinal duplication with volvulus, multiple cases across the literature report excellent outcomes with the Ladd’s procedure. However, this procedure can only take place if the segment of bowel remains viable. Additional consensus is required regarding the approach to these types of cases to enable early identification of volvulus. The differential for small bowel obstruction in an adult should include congenital malrotation leading to volvulus, as demonstrated in the cases presented. One must maintain a high index of suspicion for malrotation and minimize time to operation in order to preserve the viability of the small intestine and nutritional status of the patient.
REFERENCES
1.
Tiwari C, Shah H, Waghmare M, Makhija D, Khedkar K. Cysts of gastrointestinal origin in children: Varied presentation. Pediatr Gastroenterol Hepatol Nutr 2017;20(2):94–9. [CrossRef]
[Pubmed]

2.
Louw JH, Barnard CN. Congenital intestinal atresia; observations on its origin. Lancet 1955;269(6899):1065–7. [CrossRef]
[Pubmed]

3.
Husberg B, Salehi K, Peters T, et al. Congenital intestinal malrotation in adolescent and adult patients: A 12-year clinical and radiological survey. Springerplus 2016;5:245. [CrossRef]
[Pubmed]

4.
Sangüesa Nebot C, Llorens Salvador R, Carazo Palacios E, Picó Aliaga S, Ibañez Pradas V. Enteric duplication cysts in children: Varied presentations, varied imaging findings. Insights Imaging 2018;9(6):1097–106. [CrossRef]
[Pubmed]

5.
Barbosa L, Soares C, Póvoa AA, Maciel JP. Ileal duplication: An unusual cause of intestinal obstruction in adult life. BMJ Case Rep 2015;2015:bcr2014206638. [CrossRef]
[Pubmed]

6.
Antaki N, Abboud D, Lemmers A, Antaki F, Devière J. Acute recurrent pancreatitis secondary to the rare association of a duodenal duplication cyst and a pancreas divisum. Clin Res Hepatol Gastroenterol 2013;37(1):e32–6. [CrossRef]
[Pubmed]

7.
Zheng ZH, Huang JL, Wei HB, Liu JP, Huang Y. Adult congenital intestinal malrotation accompanied by midgut volvulus: Report of eight cases. Int J Clin Exp Med 2014;7(6):1614–8. [CrossRef]
[Pubmed]

8.
Huang ZH, Wan ZH, Vikash V, Vikash S, Jiang CQ. Report of a rare case and review of adult intestinal duplication at the opposite side of mesenteric margin. Sao Paulo Med J 2018;136(1):89–93.
[Pubmed]

9.
D’Souza J, Richards S. Enteric duplication cyst as a cause for small bowel obstruction in adulthood. N Z Med J 2018;131(1474):74–6.
[Pubmed]

10.
Cheng CL, Liu NJ, Yu MC. Intraluminal tubular duodenal duplication with bleeding. Clin Gastroenterol Hepatol 2014;12(2):e10–1. [CrossRef]
[Pubmed]

11.
Kurien RT, Chowdhury SD, Unnikrishnan LS, et al. Endoscopic treatment of a duodenal duplication cyst. Endoscopy 2014;46 Suppl 1 UCTN:E583–4. [CrossRef]
[Pubmed]

12.
Ho YC. Total colorectal and terminal ileal duplication presenting as intussusception and intestinal obstruction. World J Gastroenterol 2012;18(43):6338–40. [CrossRef]
[Pubmed]

13.
Vivier PH, Beurdeley M, Bachy B, Aguilella C, Ickowicz V, Lemoine F, Dacher JN. Ileal duplication. Diagn Interv Imaging 2013;94(1):98–100. [CrossRef]
[Pubmed]

14.
Handra-Luca A. Adult ileal duplication revealed by a colon adenoma. Surg Today 2013;43(11):1335–6. [CrossRef]
[Pubmed]

15.
Li BL, Huang X, Zheng CJ, Zhou JL, Zhao YP. Ileal duplication mimicking intestinal intussusception: A congenital condition rarely reported in adult. World J Gastroenterol 2013;19(38):6500–4. [CrossRef]
[Pubmed]

16.
Nussbaum DP, Bhattacharya SD, Jiang X, Cardona DM, Strickler JH, Blazer DG 3rd. Gastroesophageal heterotopia and HER2/neu overexpression in an adenocarcinoma arising from a small bowel duplication. Arch Pathol Lab Med 2014;138(3):428–31. [CrossRef]
[Pubmed]

17.
Kim HS, Sung JY, Park WS, Kim YW. An ileal duplication cyst manifested as an ileocolic intussusception in an adult. Turk J Gastroenterol 2014;25 Suppl 1:196–8. [CrossRef]
[Pubmed]

18.
Park JY, Her KH, Kim BS, Maeng YH. A completely isolated intestinal duplication cyst mimicking ovarian cyst torsion in an adult. World J Gastroenterol 2014;20(2):603–6. [CrossRef]
[Pubmed]

19.
Martínez-Alcalá García F, Peréz Pozo JM, Martínez-Alcalá García A, Ciria Ávila JA, Martínez Alcalá F. Duodenal duplication cyst and its endoscopic resolution]. [Article in Spanish]. Gastroenterol Hepatol 2014;37(4):274–5. [CrossRef]
[Pubmed]

20.
Kusnierz K, Pilch-Kowalczyk J, Gruszczynska K, Baron J, Lucyga M, Lampe P. A duodenal duplication cyst manifested by duodenojejunal intussusception and chronic pancreatitis. Surgery 2014;156(3):742–4. [CrossRef]
[Pubmed]

21.
Gupta A, Chakaravarthi K, Pattnaik B, Kaman L. Duplication cyst of ileum presenting as acute intestinal obstruction in an adult. BMJ Case Rep 2016;2016:bcr2016214775. [CrossRef]
[Pubmed]

22.
Yu Y, Wu JS, Ke ZW. Giant chylous cyst and ileal duplication in a young adult. Singapore Med J 2014;55(5):e77–81. [CrossRef]
[Pubmed]

23.
Furuya K, Hada M, Sugai H, et al. Gastrointestinal stromal tumor arising in an ileal duplication: Report of a case. Surg Today 2012;42(12):1234–9. [CrossRef]
[Pubmed]

24.
Miloudi N, Mzoughi Z, Ben Abid S, Sabbagh S, Arfa N, Khalfallah MT. Duodenal duplication treated surgically. [Article in French]. Tunis Med 2012;90(11):837–8.
[Pubmed]

25.
Palacios A, De Vera M, Martínez-Escoriza JC. Prenatal sonographic findings of duodenal duplication: Case report. J Clin Ultrasound 2013;41 Suppl 1:1–5. [CrossRef]
[Pubmed]

26.
Kachi A, Haddad F, Geagea A, Tohmeh MJ. Unusual case of jejunal duplication in a 64-year-old female. J Med Liban 2016;64(1):50–3. [CrossRef]
[Pubmed]

27.
Inoue K, Sakiyama T, Setoyama K, et al. Jejunal duplication in an adult presenting with hematochezia. [Article in Japanese]. Nihon Shokakibyo Gakkai Zasshi 2016;113(4):662–71. [CrossRef]
[Pubmed]

28.
Schils N, Vandecaveye V, Van Overbeke L, Laleman W. Endoscopic treatment of a symptomatic duodenal duplication cyst. Endoscopy 2018;50(7):E184–5. [CrossRef]
[Pubmed]

SUPPORTING INFORMATION
Author Contributions
Maria Eugenia Gomez - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Marie Nunez Duarte - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Rebecca Silver - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Alayna Dieter - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Guarantor of SubmissionThe corresponding author is the guarantor of submission.
Source of SupportNone
Consent StatementWritten informed consent was obtained from the patient for publication of this article.
Data AvailabilityAll relevant data are within the paper and its Supporting Information files.
Conflict of InterestAuthors declare no conflict of interest.
Copyright© 2024 Maria Eugenia Gomez et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information.