|
Clinical Image
Frontal cranioplasty using a free osteomuscular serratus anterior flap: A case report
1 Plastic, Reconstructive and Craniomaxillofacial Microsurgery Unit, Centro Hospitalar Vila Nova de Gaia/Espinho, Vila Nova de Gaia, Portugal
Address correspondence to:
Rui Casimiro
MD, Plastic, Reconstructive and Craniomaxillofacial Microsurgery Unit, Centro Hospitalar Vila Nova de Gaia/Espinho, Rua Conceição Fernandes, s/n, 4434-502 Vila Nova de Gaia,
Portugal
Message to Corresponding Author
Article ID: 100158Z12RC2025
Access full text article on other devices

Access PDF of article on other devices

How to cite this article
Casimiro R, Poleri F, Caixeiro L, Monte F, Morgado M, Costa H. Frontal cranioplasty using a free osteomuscular serratus anterior flap: A case report. J Case Rep Images Surg 2025;11(2):1–4.ABSTRACT
No Abstract
Keywords: Chronic osteomyelitis, Frontal cranioplasty, Microsurgical reconstruction, Osteomuscular serratus anterior free flap
Case Report
A 76-year-old female Caucasian patient presented with a complex clinical history following surgical resection of a large arteriovenous malformation (AVM) in the frontal region. This initial surgery was performed in 1970 via a bicoronal approach. Following the initial AVM resection, the patient experienced a postoperative intracranial infection, which necessitated two additional surgeries to manage the complication. Despite these interventions, a small punctate opening developed in the frontal region approximately three years ago, gradually enlarging over time.
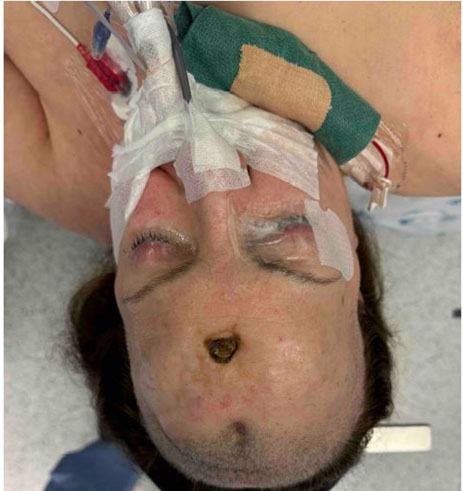
On examination, the patient exhibited exposure of the frontal bone flap due to the progressive enlargement of the punctate opening (Figure 1). No signs of neoplastic development were observed on biopsy, ruling out malignancy as a cause for the changes.
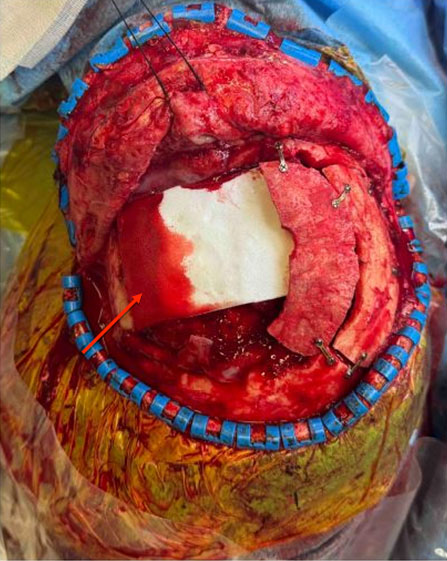
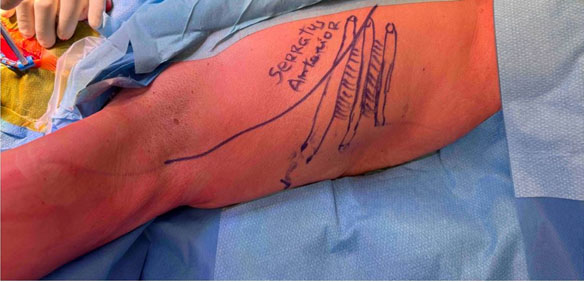
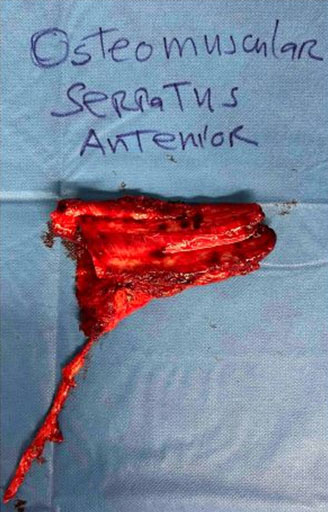
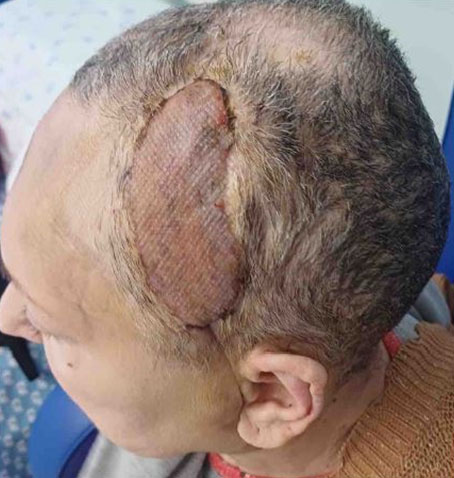
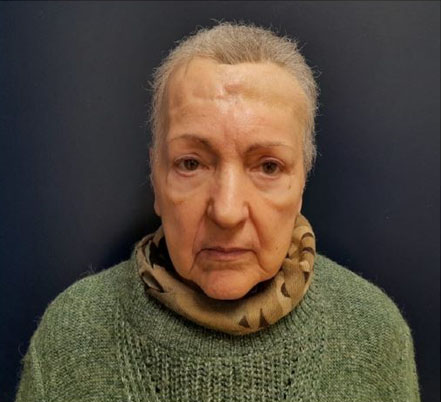
A computed tomography (CT) scan revealed an extensive area of bone erosion in the frontal region, consistent with chronic osteomyelitis. A multidisciplinary approach was chosen, involving collaboration between neurosurgery and plastic surgery teams. The patient underwent debridement and frontal craniectomy (Figure 2) and reconstruction was performed using a free osteomuscular serratus anterior flap (Figure 3) harvested from the sixth and seventh ribs (12×8 cm) (Figure 4), with the osseous component providing structural support and the muscle enhancing vascularization and tissue integration. The flap was successfully transferred using microvascular anastomosis to the facial artery and external jugular vein. Postoperative imaging with CT scan confirmed stable flap integration with minimal resorption, and the patient achieved satisfactory cosmetic and functional outcomes (Figure 5, Figure 6), with no complications such as infection, flap loss, or resorption noted over a 12-month period.
Discussion
Frontal cranioplasty is a challenging reconstructive procedure, particularly in cases involving extensive bone and soft tissue defects resulting from trauma, infection, or tumor resection [1]. Traditional reconstruction options, such as synthetic implants or autologous bone grafts, may be limited by infection risk, insufficient vascularization, or graft resorption, especially in complex cases [2]. This case report presents an alternative approach using a free osteomuscular serratus anterior flap for frontal cranioplasty in a patient with significant frontal bone loss. The serratus anterior flap offers both a robust vascular supply and adequate structural support due to its osseous component, making it a viable solution for complex cranial defects [3].
Conclusion
This case highlights the utility of the osteomuscular serratus anterior flap for complex frontal cranioplasty, emphasizing its benefits in achieving a durable, well-vascularized reconstruction in cases unsuitable for conventional techniques. Further studies are warranted to assess long-term outcomes and potential applications in various cranial reconstructive contexts.
REFERENCES
1.
Soto E, Restrepo RD, Grant JH 3rd, Myers RP. Outcomes of cranioplasty strategies for high-risk complex cranial defects: A 10-year experience. Ann Plast Surg 2022;88(5 Suppl 5):S449–54. [CrossRef]
[Pubmed]

2.
Georgeanu VA, Gingu O, Antoniac IV, Manolea HO. Current options and future perspectives on bone graft and biomaterials substitutes for bone repair, from clinical needs to advanced biomaterials research. Appl Sci 2023;13(14):8471. [CrossRef]

3.
Netscher D, Alford EL, Wigoda P, Cohen V. Free composite myo-osseous flap with serratus anterior and rib: Indications in head and neck reconstruction. Head Neck 1998;20(2):106–12. [CrossRef]
[Pubmed]

SUPPORTING INFORMATION
Author Contributions
Rui Casimiro - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Filipa Poleri - Analysis of data, Drafting the work, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Leonor Caixeiro - Analysis of data, Drafting the work, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Filipa Monte - Analysis of data, Drafting the work, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Miguel Morgado - Analysis of data, Drafting the work, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Horácio Costa - Conception of the work, Design of the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
AcknowledgmentsThe authors would like to thank Prof. Horácio Costa, senior consultant responsible for this case, for his valuable assistance and support during the preparation of this case study.
Guarantor of SubmissionThe corresponding author is the guarantor of submission.
Source of SupportNone
Consent StatementWritten informed consent was obtained from the patient for publication of this article.
Data AvailabilityAll relevant data are within the paper and its Supporting Information files.
Conflict of InterestAuthors declare no conflict of interest.
Copyright© 2025 Rui Casimiro et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information.